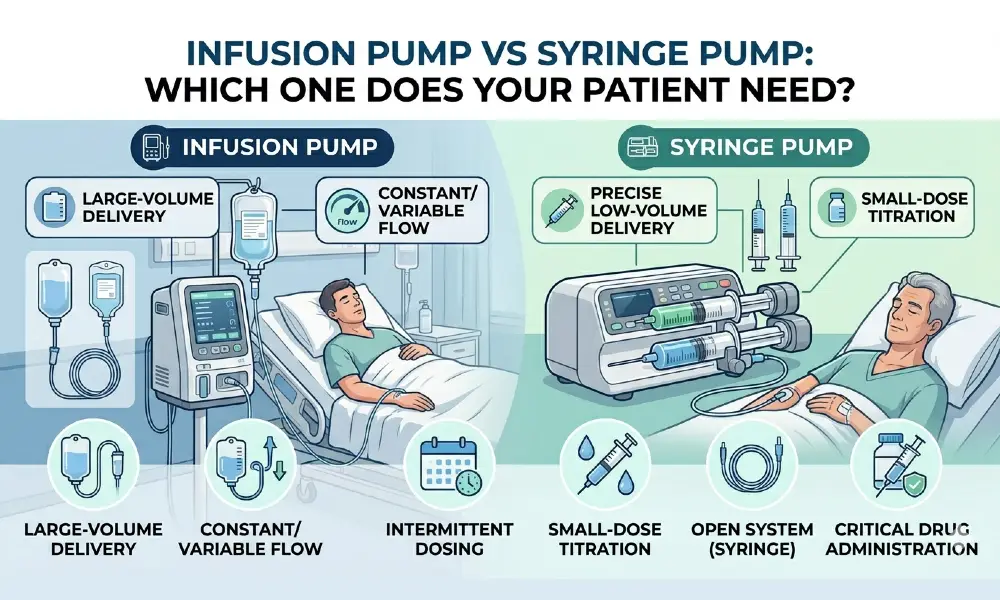
In the fast-paced world of modern healthcare, from the high-pressure environment of an Intensive Care Unit (ICU) to the specialized care in a neonatal ward, the precise delivery of fluids and medication is non-negotiable. When a patient requires intravenous (IV) therapy, clinicians often face a critical choice: Should we use a Large Volume Infusion Pump (LVIP) or a Syringe Pump?
While both devices are designed to deliver fluids into a patient’s body in controlled amounts, they are far from interchangeable. Choosing the wrong device can lead to dosing inaccuracies, delayed therapy, or even patient harm.
In this comprehensive guide, we will break down the mechanics, clinical applications, and key differences between infusion pumps and syringe pumps to help you make the best decision for your patient’s care.
1. Understanding the Large Volume Infusion Pump (LVIP)
The Large Volume Infusion Pump, often simply called an “infusion pump,” is the workhorse of the hospital ward. It is designed to move significant quantities of fluid, such as saline, nutrients, or antibiotics, over a long duration.
How It Works
Most infusion pumps utilize a peristaltic mechanism. Imagine squeezing a tube of toothpaste to move the contents forward; the pump uses rollers or linear actuators to compress the IV tubing in a wave-like motion, pushing the fluid toward the patient.
Key Characteristics:
- High Volume Capacity: Capable of delivering liters of fluid.
- Flow Rate Range: Usually ranges from 0.1 mL/hr to 999 mL/hr.
- Reservoir: Uses standard IV bags (250 mL, 500 mL, or 1000 mL).
2. Understanding the Syringe Pump
A syringe pump is a precision instrument designed for “micro-infusions.” Instead of pulling fluid from a hanging bag, the medication is drawn into a syringe, which is then placed into the pump’s driver.
How It Works
The pump features a motorized screw mechanism that pushes the syringe plunger forward at a microscopically controlled speed. This mechanical precision allows for a much smoother flow at very low rates compared to the “pulsatile” nature of a peristaltic infusion pump.
Key Characteristics:
- Low Volume Capacity: Limited by the size of the syringe (usually 1 mL to 60 mL).
- Extreme Precision: Ideal for potent drugs where even a 0.1 mL error could be dangerous.
- Minimal Dead Space: Less medication is “lost” inside the tubing.
3. The Head-to-Head Comparison: Key Differences
To choose the right tool, we must look at how these devices perform across five critical categories:
1. Volume and Capacity
The most obvious difference is scale. If a patient is severely dehydrated and needs 2 liters of Ringer’s Lactate over 24 hours, a syringe pump is impractical, you would be changing the syringe every few minutes. Conversely, if you only need to deliver 5 mL of a highly concentrated sedative, an infusion pump is overkill and wasteful.
2. Flow Rate Precision
At high flow rates (e.g., 100 mL/hr), both pumps are highly accurate. However, at “KVO” (Keep Vein Open) rates or pediatric doses (e.g., 0.5 mL/hr), the syringe pump is superior. Peristaltic pumps can have a “pulsatile” flow, meaning the fluid moves in tiny spurts. In neonates or for drugs with a short half-life, these spurts can cause fluctuations in blood pressure or sedation levels.
3. Start-up Time and Bolus Delivery
Syringe pumps generally have a faster “start-up” time. Because the mechanical drive is directly connected to the plunger, the medication begins moving almost instantly. Infusion pumps may take a moment to overcome the compliance (stretchiness) of the PVC tubing before the flow stabilizes.
4. Pressure and Occlusion Detection
Because syringe pumps use smaller tubing and syringes, they can generate higher pressures. This is vital for delivering medication through very fine-gauge needles or catheters used in pediatric care. However, it also means they are more sensitive to “occlusions” (blockages), sounding alarms quickly if a line becomes pinched.
5. Portability and Space
Syringe pumps are significantly smaller and lighter. In a crowded ICU “cockpit” where a patient might be on ten different medications, stacking five small syringe pumps is often more space-efficient than using multiple large infusion modules.
4. Clinical Use Cases: Which One for Which Patient?
Use an Infusion Pump (LVIP) For:
- Fluid Resuscitation: Replacing blood volume or treating dehydration.
- Parenteral Nutrition (TPN): Delivering liquid nutrients directly into the bloodstream.
- Routine Antibiotics: Most standard IV piggyback medications.
- General Surgery: Maintaining hydration during long procedures.
Use a Syringe Pump For:
- Neonatal and Pediatric Care: Where fluid overload is a constant risk and doses are tiny.
- Vasoactive Medications: Drugs like Norepinephrine or Dopamine that require second-to-second precision.
- Anesthesia and Sedation: Maintaining a steady state of “sleep” during surgery or mechanical ventilation.
- Pain Management (PCA): Patient-Controlled Analgesia, where small, concentrated doses of opioids are delivered.
5. Safety Features: The “Smart Pump” Revolution
Regardless of the type, modern pumps are now “Smart Pumps.” They are equipped with Dose Error Reduction Systems (DERS).
- Drug Libraries: Clinicians select the specific drug from a pre-programmed list.
- Hard and Soft Limits: If a nurse accidentally types 100 mL/hr instead of 10 mL/hr for a dangerous drug, the pump will “alarm” and refuse to start.
- Connectivity: Modern pumps sync with Electronic Health Records (EHR) to ensure the right patient gets the right dose.
6. Maintenance and Cost Considerations
From a facility management perspective, the two pumps represent different investments.
| Feature | Infusion Pump (LVIP) | Syringe Pump |
|---|---|---|
| Initial Cost | Moderate to High | Moderate |
| Consumables | Expensive (Proprietary IV sets) | Lower (Standard syringes/tubing) |
| Maintenance | Requires regular calibration of rollers | Requires lubrication of the lead screw |
| Versatility | High (Can do almost anything) | Low (Specialized for small volumes) |
7. Troubleshooting Common Problems
Air-in-Line (Infusion Pumps)
Peristaltic pumps are prone to “Air-in-Line” alarms. Because they pull from large bags, air bubbles can easily enter the system. This requires “priming” the line carefully—a step that is often simpler with syringe pumps where air can be manually flicked out of the syringe before loading.
Occlusion Alarms (Syringe Pumps)
Because syringe pumps are so precise, they are sensitive. A patient simply bending their arm can trigger a high-pressure alarm. Clinicians must ensure that the “pressure limit” settings are appropriate for the patient’s catheter size to avoid “nuisance alarms.”
Wrapping Up
Choosing between an infusion pump and a syringe pump boils down to two questions: How much fluid is being delivered? And How dangerous is a small dose error?
Choose the Infusion Pump for bulk fluid, nutrition, and standard medications where the volume exceeds 60 mL.
Choose the Syringe Pump for critical care, pediatrics, and high-potency drugs where precision is life-critical.
By matching the device to the clinical need, healthcare providers can ensure maximum patient safety and therapeutic efficacy.
Frequently Asked Questions
Q1. Can I use a syringe pump for a blood transfusion?
Generally, no. Blood cells can be damaged (hemolysis) if forced through the small-bore tubing and high pressures often associated with syringe pumps. Large-volume infusion pumps or dedicated blood warmers/infusers are preferred.
Q2. Why do syringe pumps beep more often than infusion pumps?
They are more sensitive to pressure changes. Because they are often used with very thin catheters, any slight movement or kink in the line causes a pressure spike that triggers the safety alarm.
Q3. Is there a “Universal” pump?
While some modular systems allow you to attach both infusion and syringe “heads” to a single “brain,” the mechanical delivery methods remain distinct to suit different clinical needs.
Don’t Miss: Auto BiPAP Vs Fixed BiPAP: Which Technology Provides Better Sleep Quality?